Psychosomatic theory attempts to explain how subjective emotional experiences are translated into measurable physiological phenomena. At the core of this inquiry lies a central problem: emotional states are abstract, internally experienced, and often difficult to articulate, yet they can produce concrete, observable disturbances across multiple biological systems. This transformation—from affect to symptom—is neither linear nor simplistic. It involves layered interactions between neural processing, autonomic regulation, cognitive interpretation, and learned patterns of response. Understanding how emotions become symptoms requires examining the pathways through which affective processes are encoded, regulated, and expressed within the organism.
Emotions are not isolated events; they are complex, multi-component processes involving appraisal, physiological activation, expressive behavior, and subjective feeling. When an individual encounters a stimulus, it is evaluated in terms of relevance, threat, or significance. This appraisal initiates coordinated changes across neural and physiological systems, preparing the organism to respond. These changes include shifts in cardiovascular activity, muscle tone, endocrine signaling, and attentional focus.
Under typical conditions, emotional responses are transient and adaptive. Once the stimulus is resolved, regulatory mechanisms restore equilibrium. However, when emotional processing is disrupted—due to chronic stress, unresolved conflict, or impaired regulation—these responses may persist or recur in maladaptive ways. It is within this context that emotional states begin to manifest as physical symptoms.
One of the primary mechanisms underlying this transformation is autonomic dysregulation. The autonomic nervous system mediates involuntary physiological functions and plays a central role in emotional expression. Repeated or prolonged activation can lead to sustained patterns of physiological arousal. Over time, these patterns may become ingrained, producing symptoms such as tension, discomfort, or functional disturbance in various organ systems.
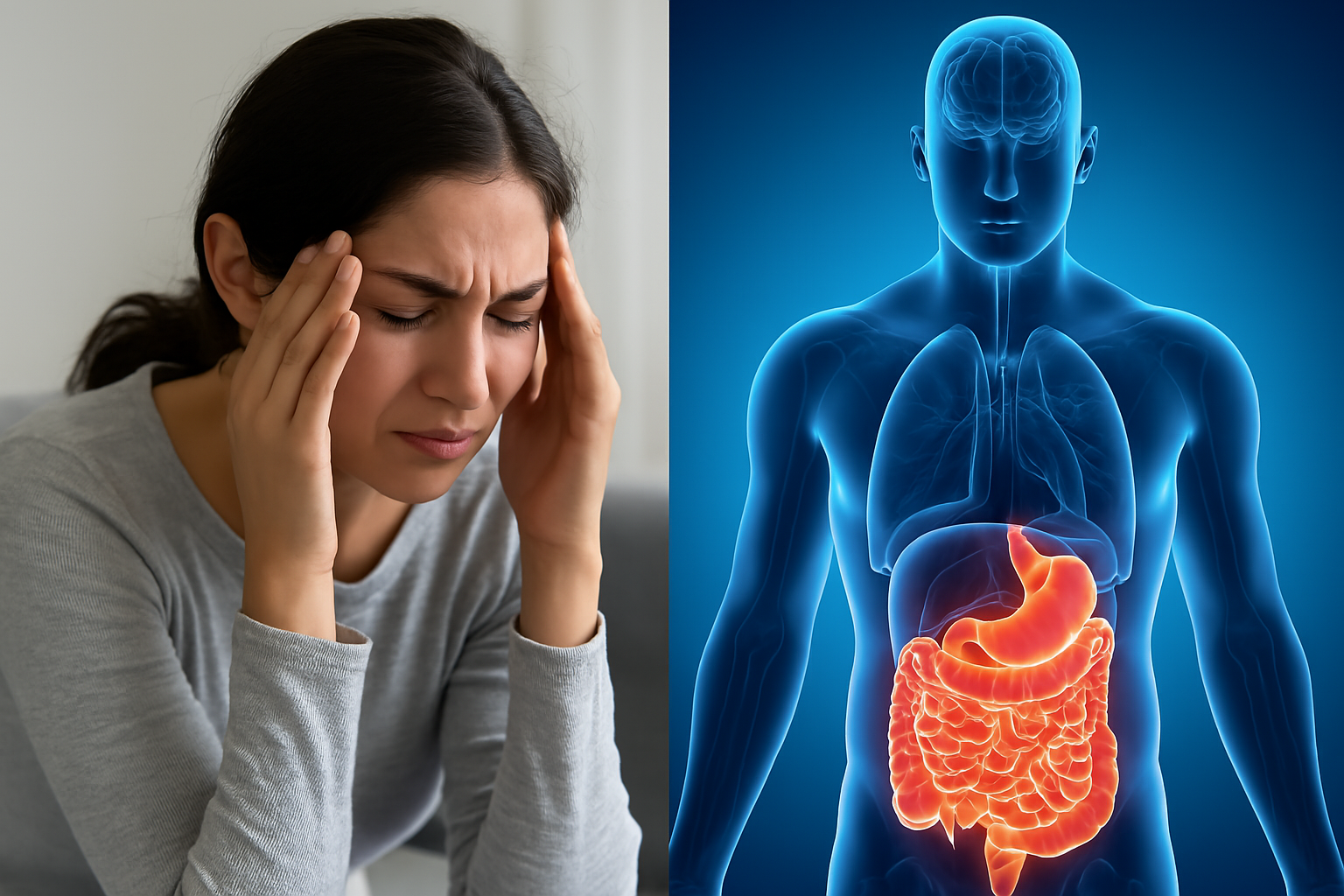
Importantly, these symptoms are not random. They often follow pathways shaped by individual vulnerability, past experience, and contextual factors. For example, one individual may consistently experience gastrointestinal discomfort under stress, while another develops musculoskeletal pain. These patterns suggest that emotional expression through physiological channels is influenced by both biological predispositions and learned associations.
Interoception—the perception of internal physiological states—further mediates this process. Individuals vary in their sensitivity to internal signals, as well as in how they interpret them. Heightened interoceptive awareness can amplify the perception of minor fluctuations, transforming them into salient experiences. When combined with anxious or catastrophic interpretations, this amplification can intensify symptoms and reinforce their persistence.
Cognitive appraisal plays a critical role in determining whether physiological sensations are experienced as benign or threatening. When sensations are interpreted as signs of dysfunction or danger, they may trigger additional emotional responses, such as anxiety or fear. These responses, in turn, increase physiological activation, creating a feedback loop that sustains and magnifies symptoms.
Memory contributes to the stabilization of these patterns. Repeated pairings of emotional states with specific physiological responses can lead to associative learning. Over time, certain contexts or thoughts may automatically trigger both emotional and physical reactions, even in the absence of an immediate external stressor. This learned coupling can make symptoms appear spontaneous or inexplicable from the individual’s perspective.
Trauma introduces additional complexity into the transformation of emotion into symptom. Traumatic experiences often involve overwhelming affect that cannot be fully processed or integrated. As a result, elements of the experience may be stored in fragmented forms—sensory, affective, or procedural—rather than as coherent narratives. These fragments can later be reactivated, producing physiological responses that are disconnected from conscious awareness of their origin.
In such cases, symptoms may represent implicit expressions of unresolved emotional material. The organism responds as though the original threat were present, even when the current environment is safe. This mismatch between context and response contributes to the persistence and intensity of psychosomatic symptoms.
The role of language and symbolic processing is also significant. Emotions that are not adequately symbolized—meaning they are not translated into words or concepts—may be more likely to be expressed through physiological channels. This phenomenon suggests that the ability to articulate and reflect upon emotional states can influence how they are manifested. When symbolic processing is limited, the burden of expression may shift toward somatic pathways.
Cultural and social factors shape this process by influencing how emotions are recognized, expressed, and valued. In some contexts, direct expression of emotional distress may be discouraged, leading individuals to communicate distress through physical symptoms. These expressions may be more socially acceptable or more likely to elicit support, reinforcing their use as communicative signals.
Neurobiologically, the integration of emotional and physiological processes involves multiple interconnected systems. Regions involved in affective processing interact with those responsible for regulation and bodily control. These interactions allow emotional states to influence physiological activity, while feedback from physiological systems informs emotional experience.
Hormonal pathways also contribute to the embodiment of emotion. Stress-related hormones affect numerous physiological processes, including immune function, metabolism, and cardiovascular regulation. Chronic activation of these pathways can lead to persistent changes that underlie many psychosomatic conditions.
The immune system, in particular, demonstrates sensitivity to emotional states. Psychological stress can alter immune responses, contributing to inflammation or susceptibility to illness. This interaction underscores the extent to which emotional processes can influence biological functioning at a systemic level.
Despite the complexity of these mechanisms, the emergence of symptoms often follows recognizable patterns. Emotional overload, lack of regulation, and persistent cognitive focus on distress can converge to produce stable symptom profiles. These profiles may become part of the individual’s experience of self, further reinforcing their persistence.
It is important to emphasize that psychosomatic symptoms are genuine physiological experiences. They are not fabricated or imagined, even when their origins involve psychological processes. The distinction lies not in the reality of the symptoms but in the pathways through which they arise.
Clinical approaches to psychosomatic conditions focus on disrupting maladaptive patterns and restoring integration. This may involve enhancing emotional awareness, modifying cognitive appraisals, and reducing physiological activation. Techniques that promote regulation—such as controlled breathing, relaxation, and mindfulness—can help recalibrate autonomic responses.
Cognitive interventions aim to alter interpretations of physiological sensations, reducing the tendency to view them as threatening. By changing the meaning assigned to these sensations, individuals can break the feedback loops that sustain symptoms. Over time, this can lead to a reduction in both the intensity and frequency of symptoms.
Emotional processing is equally important. Facilitating the recognition and expression of emotions can reduce the need for physiological expression. When emotional experiences are integrated into conscious awareness and symbolic frameworks, their impact on physiological systems may diminish.
The concept of plasticity provides a hopeful perspective on these processes. Just as emotional patterns can become embodied, they can also be modified. The systems involved in psychosomatic expression are dynamic and responsive to change. Through targeted interventions and supportive environments, individuals can develop more adaptive patterns of regulation.
Ultimately, the transformation of emotions into symptoms reflects the interconnected nature of psychological and physiological processes. Emotions do not remain confined to subjective experience; they are translated into patterns of activation that can influence multiple systems. When these patterns become dysregulated, they may manifest as persistent symptoms.
This transformation is not a failure of the organism but a reflection of its attempt to adapt to complex and often overwhelming conditions. Symptoms can be understood as signals—indications that underlying processes require attention and integration. By attending to these signals, it becomes possible to address the roots of distress rather than merely its manifestations.
In this sense, emotions become symptoms when the pathways of regulation, interpretation, and integration are disrupted. The organism expresses what cannot be fully processed through other means, converting affect into physiological experience. Understanding this process provides a framework for both explaining and addressing the intricate relationship between emotion and symptom formation.