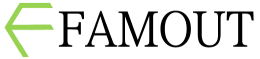Daily commuting is a routine part of life for millions of people around the world, but its psychological impact is often underestimated. Long hours spent traveling to and from work—whether by car, bus, train, or other means—can significantly affect mental health and overall well-being. One of the primary stressors associated with commuting is the loss of personal time. When individuals spend one to three hours each day in transit, they have less time for rest, family, hobbies, and self-care. Over time, this time deficit can contribute to chronic fatigue, irritability, and a diminished quality of life. Traffic congestion is another major factor in commuter stress. Being stuck in slow-moving traffic can cause frustration, increase blood pressure, and trigger feelings of helplessness. Similarly, crowded public transportation systems can create sensory overload and raise anxiety levels, particularly for individuals with claustrophobia or social anxiety. The unpredictability of travel times also adds to the psychological burden. Delays caused by accidents, weather, or mechanical issues can heighten feelings of stress, especially for those with strict work schedules. This unpredictability often forces commuters to leave earlier than necessary, further reducing their free time. Research has shown that long commutes are linked to higher rates of depression, anxiety, and even sleep disturbances. Physical health can also suffer, as prolonged sitting contributes to back pain, poor posture, and decreased cardiovascular fitness. In some cases, the mental and physical toll of commuting can lead to burnout and reduced job satisfaction. To mitigate these effects, experts suggest strategies such as flexible working hours, remote work opportunities, and alternative transportation methods like cycling or walking for part of the journey. Mindfulness techniques, audiobooks, or music can make the commute more tolerable, while employers can help by offering hybrid work models or transportation subsidies. In conclusion, commuting is more than just a logistical necessity—it is a daily experience that shapes mental health in profound ways. By acknowledging and addressing commuter stress, both individuals and organizations can foster healthier, more balanced lifestyles.
Digital Nomad Lifestyle and Mental Health
In recent years, the rise of remote work has created a new category of professionals known as “digital nomads.” These individuals use technology to work from anywhere in the world, often traveling frequently while maintaining online jobs. While this lifestyle offers unparalleled freedom and flexibility, it also presents unique mental health challenges that are often overlooked. One of the primary benefits of the digital nomad lifestyle is the autonomy it provides. The ability to choose one’s working environment, avoid daily commutes, and experience different cultures can lead to higher levels of satisfaction and personal growth. However, the constant movement can disrupt stability and routines, both of which are important for mental well-being. Loneliness is a common issue among digital nomads. Without a consistent social network, individuals may struggle to form meaningful, long-term connections. This transient lifestyle can lead to feelings of isolation, particularly when traveling to countries where language barriers make communication difficult. Over time, this can increase vulnerability to depression and anxiety. Another psychological challenge is the blurring of boundaries between work and personal life. Working from cafes, hostels, or temporary apartments can make it difficult to “switch off” from professional responsibilities. The pressure to be constantly available online can contribute to burnout, even if the physical setting appears relaxed. Financial uncertainty is another stressor. Many digital nomads work as freelancers or run small online businesses, meaning income can fluctuate dramatically from month to month. This instability can create chronic stress, particularly if unexpected expenses arise while abroad. To maintain mental health in this lifestyle, experts recommend building routines regardless of location, engaging in local communities, setting clear work hours, and prioritizing regular communication with family and friends. Practices such as mindfulness, exercise, and periodic “digital detoxes” can also help prevent burnout. While the digital nomad lifestyle offers adventure and personal freedom, it is not without its psychological costs. Balancing exploration with stability is essential for sustaining both mental well-being and professional success over the long term.
Childhood Trauma and Mental Health
Childhood trauma, which includes experiences such as physical, emotional, or sexual abuse, neglect, and exposure to violence, has far-reaching effects on an individual’s mental health throughout life. These early adverse experiences can disrupt normal brain development, particularly in areas responsible for emotional regulation and stress response like the amygdala, hippocampus, and prefrontal cortex. Such neurobiological changes contribute to heightened emotional sensitivity, difficulties in managing stress, and impaired cognitive functions. Psychologically, individuals who have experienced childhood trauma often struggle with emotional regulation, exhibit increased impulsivity, and may engage in risk-taking behaviors such as substance abuse. Interpersonal relationships may suffer due to attachment issues, mistrust, and difficulty in forming healthy bonds. The impact of unresolved childhood trauma can extend into adulthood, increasing the risk of developing psychiatric disorders including depression, anxiety, post-traumatic stress disorder (PTSD), and personality disorders. Early identification and intervention are crucial to help mitigate these negative outcomes. Trauma-informed therapeutic approaches such as cognitive-behavioral therapy (CBT), eye movement desensitization and reprocessing (EMDR), and family therapy have demonstrated effectiveness in addressing trauma symptoms and fostering resilience. Additionally, community and family support play a vital role in the recovery process. Preventive measures focus on creating safe environments, educating caregivers, and improving parenting practices to reduce the incidence of childhood trauma. Public awareness campaigns and reducing stigma around mental health are also essential to encourage affected individuals to seek help without fear of judgment. In conclusion, childhood trauma is a significant factor influencing mental health across the lifespan. Addressing its effects requires a comprehensive, multidisciplinary approach that incorporates psychological, social, and biological perspectives to promote healing and improve quality of life.
Sleep Disorders and Mental Health: Interactions, Consequences, and Contemporary Approaches
Sleep disorders represent a growing public health concern worldwide, significantly impacting mental health and overall well-being. Conditions such as insomnia, sleep apnea, restless leg syndrome, and circadian rhythm disruptions not only impair sleep quality but also contribute to the development and exacerbation of various psychiatric disorders, including depression, anxiety, bipolar disorder, and cognitive decline. The bidirectional relationship between sleep and mental health is well-documented: poor sleep can increase vulnerability to psychological problems, while mental health disorders can further disrupt sleep patterns, creating a vicious cycle. Neurochemical imbalances caused by inadequate sleep affect brain regions responsible for emotional regulation and cognitive functions, leading to symptoms such as mood swings, irritability, impaired concentration, and memory difficulties. The COVID-19 pandemic has intensified these challenges by increasing stress levels and social isolation, resulting in a marked rise in sleep disturbances globally. Many individuals report difficulty falling asleep, fragmented sleep, or non-restorative sleep, which further aggravates anxiety and depressive symptoms. Effective management of sleep disorders involves a comprehensive approach. Behavioral interventions like Cognitive Behavioral Therapy for Insomnia (CBT-I) have shown strong efficacy by addressing maladaptive thoughts and behaviors related to sleep. Emphasis on sleep hygiene—including maintaining a regular sleep schedule, creating a restful environment, and limiting screen time before bed—is fundamental. In some cases, pharmacological treatments are necessary to support recovery, though they are generally recommended for short-term use due to potential side effects. Increasing public awareness about the critical role of sleep in mental health is vital for early detection and intervention. Healthcare providers must consider sleep assessments as an integral part of psychiatric evaluation to tailor treatment plans effectively. Furthermore, ongoing research into the neurobiological mechanisms linking sleep and mental health will continue to enhance therapeutic strategies. In summary, sleep disorders and mental health are intricately connected, with disruptions in one domain often leading to challenges in the other. Addressing sleep problems proactively can significantly improve psychological well-being, cognitive performance, and quality of life, underscoring the importance of integrated care in mental health services.
Pandemic Aftermath and Its Impact on Mental Health
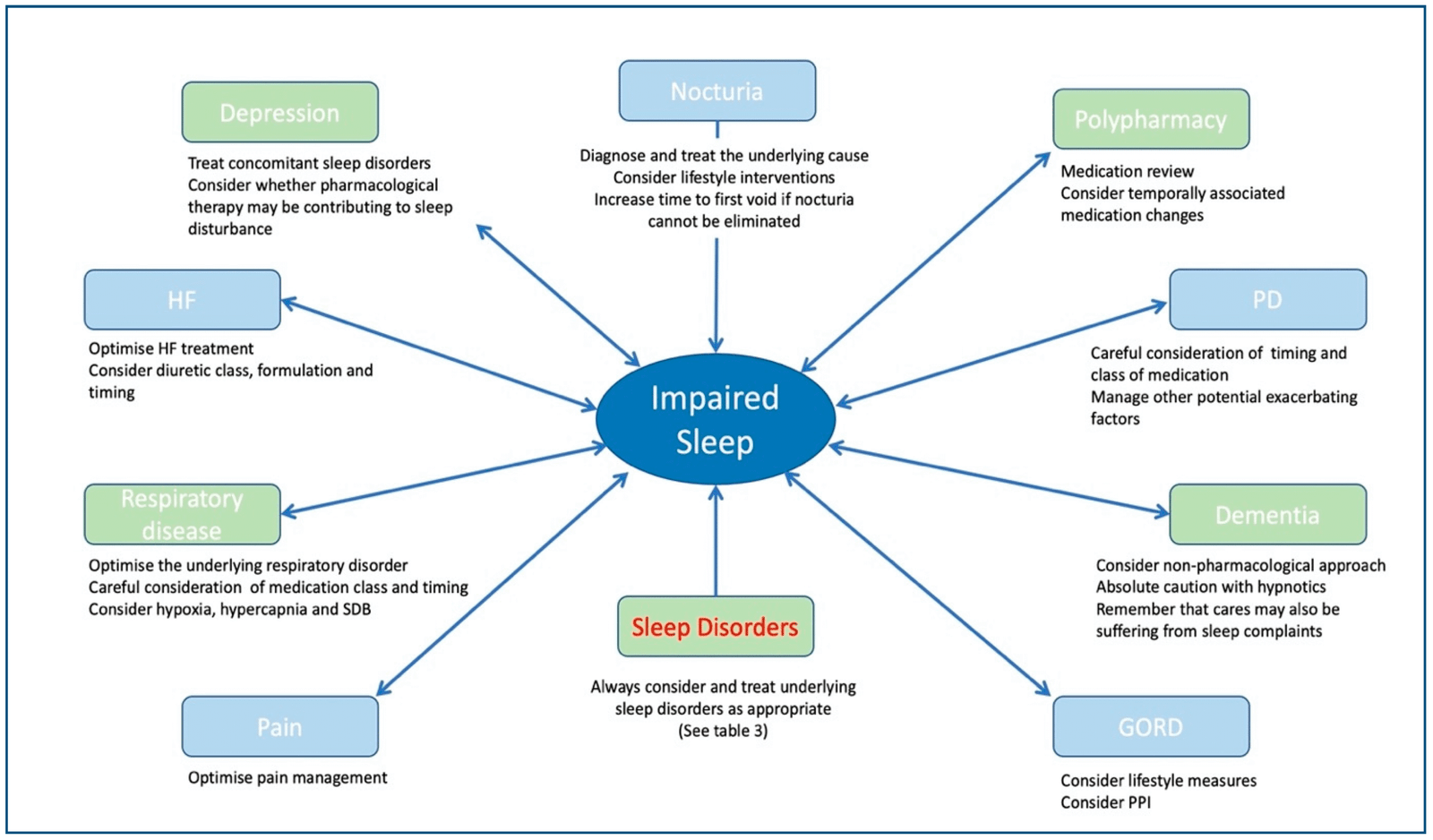
The COVID-19 pandemic has profoundly affected global mental health, leading to an unprecedented rise in psychological disorders such as anxiety, depression, and post-traumatic stress disorder (PTSD). Social isolation, economic uncertainty, grief from loss, and disruptions to daily life have contributed to increased stress levels and emotional distress across all age groups. Healthcare workers and vulnerable populations have experienced heightened risks of burnout and trauma. Moreover, the pandemic accelerated the adoption of teletherapy and digital mental health solutions, which have improved access but also highlighted disparities in care. Addressing the long-term psychological effects of the pandemic requires comprehensive strategies involving community support, accessible mental health services, and policies aimed at reducing stigma and promoting resilience.
Attention Deficit Hyperactivity Disorder (ADHD) in Adults: A Current Overview
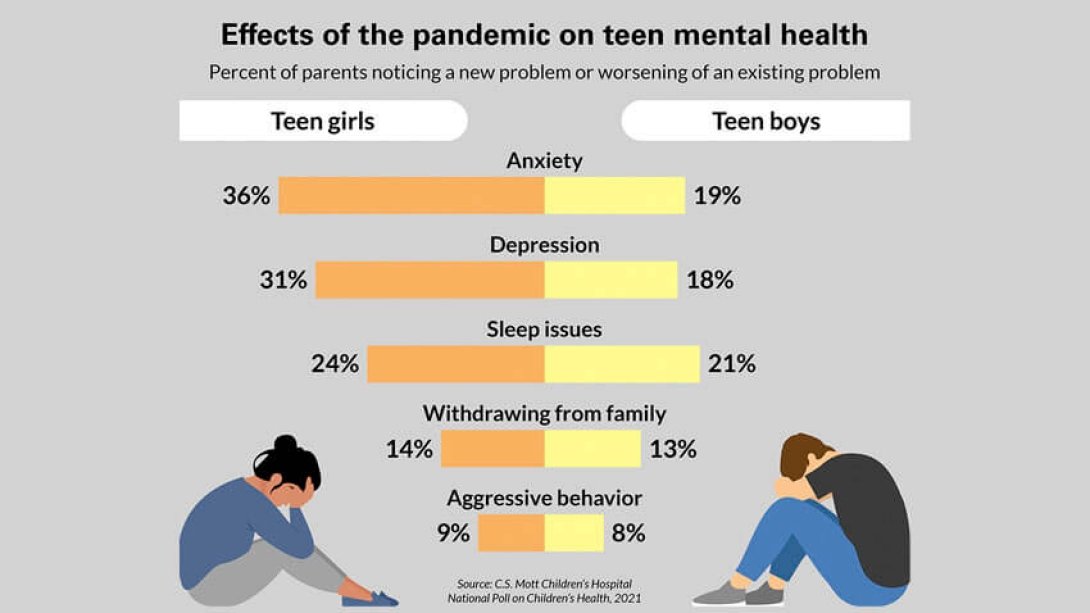
Attention Deficit Hyperactivity Disorder (ADHD) is traditionally known as a neurodevelopmental disorder that emerges in childhood, but its symptoms can persist into adulthood or may be diagnosed later in life. Adult ADHD is characterized by core symptoms such as inattention, hyperactivity, and impulsivity, which can significantly impact an individual’s daily quality of life. The most common symptoms in adults include difficulties sustaining attention, challenges with organization and planning, forgetfulness, internal restlessness, and impulsive behaviors. Unlike childhood hyperactivity, which is often seen as excessive physical movement, adult hyperactivity more commonly presents as internal feelings of restlessness. Impulsivity may manifest as hasty decision-making, impatience, and uncontrolled behaviors in social settings. In recent years, the widespread use of technology and the constant demands of digital environments have contributed to a higher visibility of ADHD symptoms in adults. Social media use, multitasking requirements, and fast-paced lifestyles can exacerbate attention difficulties and intensify the disorder’s effects. Additionally, increased awareness of ADHD has led to better recognition of previously overlooked cases. Diagnosis of adult ADHD involves clinical interviews and assessing whether symptoms have been present since childhood. Differential diagnosis is crucial because ADHD often coexists with other psychiatric conditions such as anxiety and depression. Treatment typically combines medication (including stimulants and non-stimulants) with psychotherapy methods like cognitive-behavioral therapy. Lifestyle changes, such as regular exercise, maintaining healthy sleep patterns, and limiting digital device use, also play a supportive role in managing symptoms. Adult ADHD can be effectively managed with early diagnosis and appropriate treatment. If left untreated, it can negatively affect work performance, social relationships, and emotional stability. Therefore, evaluating adults who struggle in their professional or social lives for ADHD is essential. In conclusion, adult ADHD has become an increasingly recognized health concern. Enhancing clinical and social awareness, improving access to treatment, and developing supportive strategies will contribute to improving the quality of life for those affected.
Decision-Making Psychology
Decision-making is a fundamental psychological process that shapes human behavior and influences outcomes in nearly every aspect of life. From minor daily choices to complex and high-stakes decisions, the ways in which individuals gather information, evaluate options, and select actions reveal much about human cognition, motivation, and emotion. Classical decision-making theories often assume that humans are rational agents who aim to maximize benefits and minimize costs through logical reasoning. This perspective is exemplified by Rational Choice Theory, which suggests that individuals weigh all possible options, assess their probable outcomes, and choose the one with the highest expected utility. However, extensive research in cognitive psychology shows that human decision-making frequently deviates from this ideal due to cognitive biases, limited information, and emotional influences. Psychologist Daniel Kahneman and his collaborator Amos Tversky demonstrated through their work on prospect theory that people systematically violate the principles of rationality when making decisions under risk and uncertainty. For example, individuals tend to overweigh potential losses compared to equivalent gains, a phenomenon known as loss aversion. This helps explain why people sometimes hold onto failing investments or avoid taking necessary risks. Another important concept in decision-making research is the role of heuristics—mental shortcuts that simplify complex judgments. While heuristics can make decision-making more efficient, they can also lead to predictable errors. For example, the availability heuristic causes people to judge the likelihood of events based on how easily examples come to mind, which can distort risk perception. Similarly, the anchoring effect shows that initial information can heavily influence final decisions, even when it is irrelevant. Emotions play a significant role in how people make choices. The affect heuristic describes how feelings and immediate emotional reactions can shape judgments, often bypassing deliberate analysis. This means that mood, stress, and prior experiences all interact with cognitive processes, sometimes speeding up decisions but sometimes introducing bias. Individual differences also influence decision-making styles. Some people prefer analytical, systematic approaches, while others rely more on intuition or gut feelings. Personality traits such as impulsivity, need for closure, and tolerance for ambiguity affect how decisions are approached and executed.
The Psychology of Psychological Boundaries
Psychological boundaries are the invisible lines that define an individual’s sense of self, personal space, and emotional limits in relation to others. Healthy boundaries are essential for maintaining autonomy, protecting mental well-being, and fostering respectful and balanced relationships. When boundaries are clear and assertively communicated, they help individuals navigate social interactions without losing their sense of identity or being overwhelmed by the demands of others. Psychological research identifies boundaries as both internal and external constructs. Internal boundaries relate to regulating one’s own thoughts, emotions, and impulses, while external boundaries involve how one interacts with the surrounding environment, including family, friends, colleagues, and broader social systems. Problems arise when boundaries are either too rigid or too porous. Rigid boundaries may lead to emotional isolation, difficulties in forming close relationships, and a tendency to avoid vulnerability or trust. On the other hand, overly porous boundaries can result in people-pleasing, difficulty saying no, emotional exhaustion, and susceptibility to manipulation or exploitation. Poor boundary awareness is often linked to childhood experiences, where family dynamics, cultural norms, or past trauma may have modeled unhealthy relational patterns. The concept of assertiveness is closely tied to maintaining healthy boundaries. Assertiveness allows individuals to express their needs, preferences, and limits clearly and respectfully without infringing on others’ rights. Research shows that assertive communication skills are associated with higher self-esteem, reduced stress, and more satisfying relationships. Therapeutic approaches, including cognitive-behavioral therapy and boundary-setting training, help individuals recognize boundary violations and develop skills to reinforce their limits. Mindfulness and self-awareness practices also play a crucial role by enabling people to detect when their boundaries are being crossed and to respond proactively rather than reactively. Cultivating healthy psychological boundaries is not about building walls but about creating flexible, adaptive spaces that protect well-being while allowing for genuine connection and mutual respect. In an increasingly interconnected world where technology can blur lines between personal and professional life, the ability to maintain clear boundaries has become even more critical for sustaining mental and emotional health. In conclusion, strong psychological boundaries are a cornerstone of emotional resilience and relational balance. By understanding, communicating, and respecting these limits, individuals can foster healthier interactions, preserve their sense of self, and navigate the complexities of social life with greater confidence and well-being.
The Psychology of Self-Criticism
Self-criticism is a pervasive psychological phenomenon in which individuals evaluate themselves harshly, focusing on perceived flaws, failures, or shortcomings. While a moderate level of self-evaluation can promote personal growth by highlighting areas for improvement, excessive self-criticism often becomes a barrier to psychological well-being and healthy functioning. Psychologists distinguish between constructive self-reflection and destructive self-criticism. Constructive self-reflection is reality-based and goal-oriented, encouraging people to learn from mistakes and adjust their behavior. In contrast, self-criticism is often rigid, harsh, and emotionally charged, involving global negative judgments about one’s character or worth rather than specific behaviors. Research has linked high levels of self-critical thinking to increased risk for depression, anxiety, perfectionism, and low self-esteem. Individuals who are highly self-critical tend to magnify minor errors, interpret setbacks as personal failures, and ruminate excessively on negative self-beliefs. This cycle can erode motivation, hinder performance, and damage relationships, as self-critical individuals may project their harsh standards onto others or withdraw to avoid perceived judgment. Several factors contribute to the development of self-critical tendencies. Early experiences with overly demanding or critical caregivers, perfectionistic family environments, or chronic exposure to unrealistic social standards can shape a person’s inner narrative. Cultural norms that emphasize achievement, competition, or external validation can further reinforce the habit of harsh self-evaluation. Neuroscientific research indicates that self-critical thoughts activate brain regions associated with threat and negative affect, such as the amygdala and the medial prefrontal cortex. This explains why self-criticism is often accompanied by physiological stress responses, including tension, fatigue, or sleep disturbances. Addressing self-criticism requires intentional psychological work. One of the most effective approaches is cultivating self-compassion, which involves treating oneself with the same kindness and understanding offered to a friend in distress. Studies by researchers like Kristin Neff have shown that self-compassion reduces the impact of self-criticism and enhances resilience, emotional well-being, and motivation. Cognitive-behavioral therapy (CBT) techniques can also help individuals identify and challenge distorted self-critical thoughts, replacing them with more balanced and realistic self-assessments. In conclusion, while self-criticism may seem like a motivator for self-improvement, excessive and rigid self-judgment often undermines mental health and personal growth. Developing a compassionate, realistic, and flexible self-relationship is a crucial step toward sustainable well-being and authentic self-worth.
The Psychology of Shame
Shame is a deeply social and self-conscious emotion that arises when individuals perceive themselves as fundamentally flawed, unworthy, or unacceptable in the eyes of others. Unlike guilt, which focuses on specific behaviors that violate one’s moral standards, shame is more pervasive and tied to one’s sense of self, often resulting in feelings of exposure, inadequacy, and a desire to hide. Psychologists distinguish shame from related emotions such as guilt, embarrassment, and humiliation. While guilt can motivate reparative actions—encouraging individuals to make amends for their mistakes—shame tends to evoke withdrawal, self-condemnation, and isolation. Research by scholars like Brené Brown highlights that persistent shame is strongly correlated with anxiety, depression, low self-esteem, and a host of maladaptive coping behaviors. The roots of shame often lie in early social experiences. Families, schools, and cultural environments that use shaming as a method of control or discipline may inadvertently cultivate chronic feelings of unworthiness. Children who grow up in environments where mistakes are met with harsh criticism rather than constructive guidance are more likely to internalize the belief that they are inherently defective. Neuroscientific studies show that shame activates regions of the brain associated with social pain and threat detection, reinforcing the intense discomfort and physiological stress that accompany this emotion. To cope, individuals may engage in avoidance, perfectionism, or aggression to protect their sense of self from further exposure. Despite its painful nature, shame can be mitigated through conscious psychological work. One of the most effective antidotes is self-compassion, which involves treating oneself with kindness and understanding rather than harsh judgment. Building secure, non-judgmental relationships also creates safe spaces where individuals feel accepted despite their flaws. Therapeutic approaches such as emotion-focused therapy and shame resilience training help individuals recognize and name shame, break the cycle of secrecy, and transform self-criticism into self-acceptance. In conclusion, shame is a powerful emotion with significant implications for mental health and social connection. Understanding its origins, distinguishing it from guilt, and developing strategies to build resilience against shame are essential steps toward fostering psychological well-being and authentic self-worth.