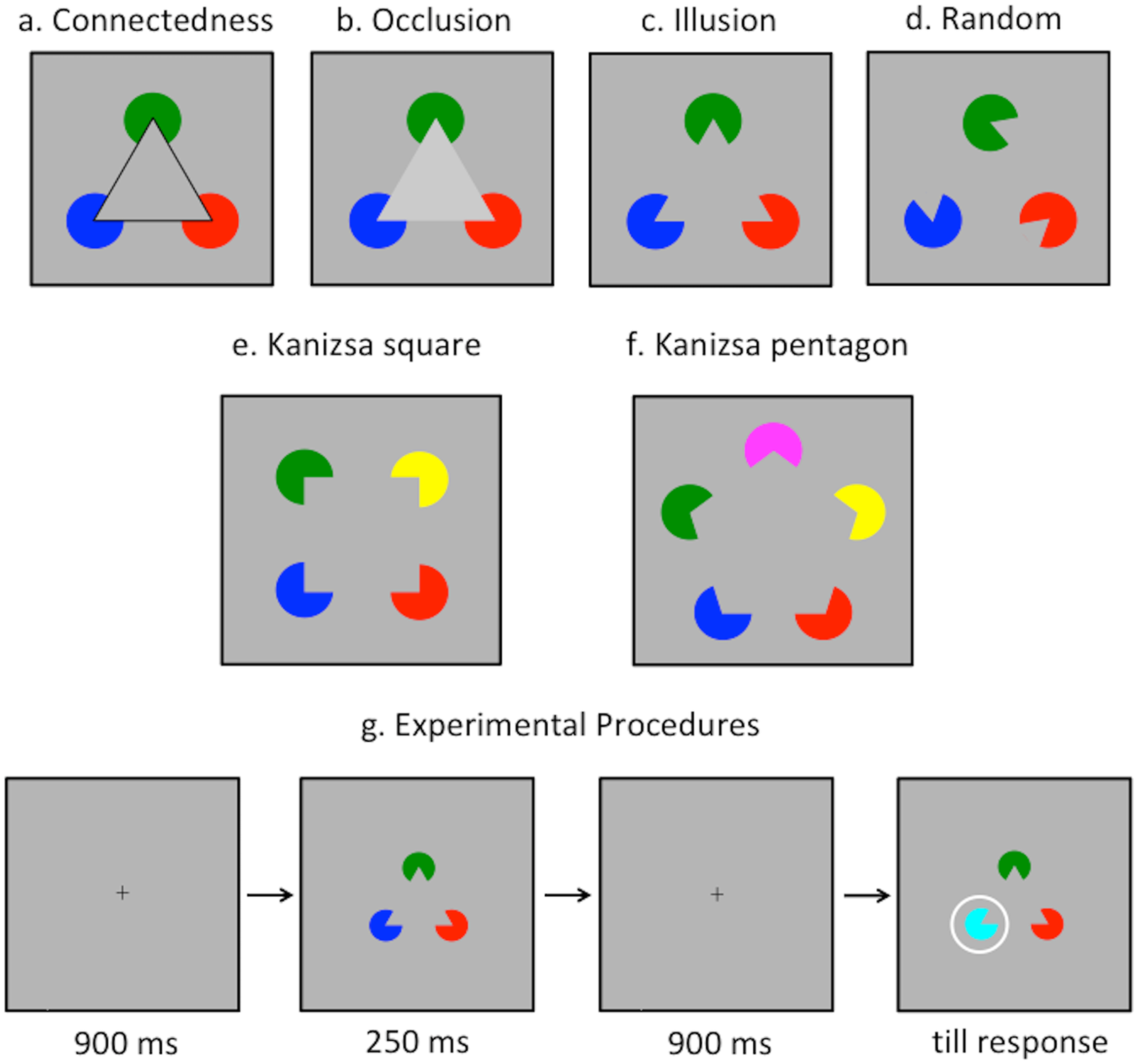
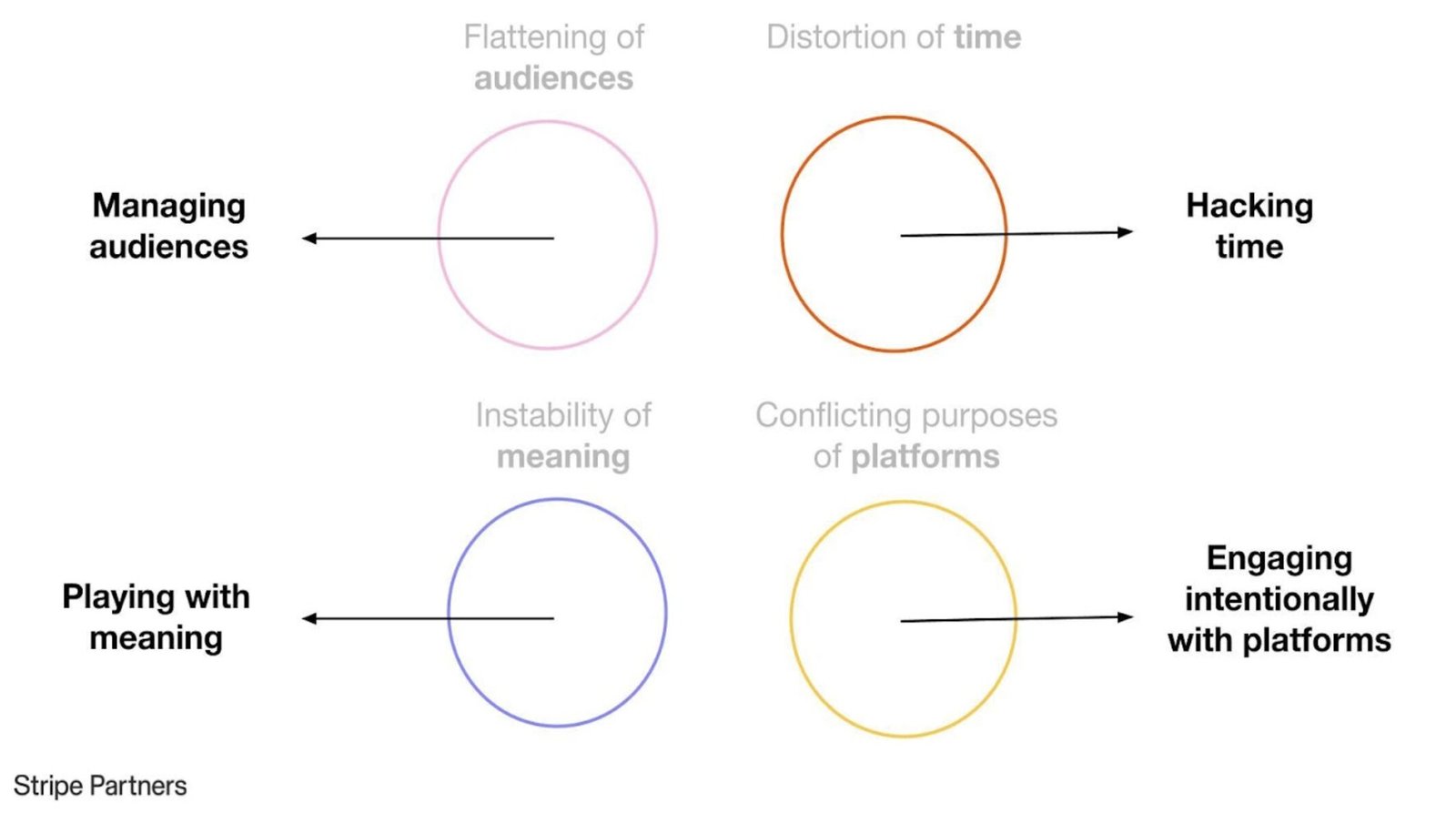
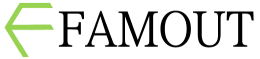Psychiatric theory often associates perceptual disturbance with distortion, hallucination, or instability. Yet an inverse and rarely described condition exists in which perception becomes excessively stable. This phenomenon, which may be termed Perceptual Over-Integrity, occurs when sensory reality is experienced as too consistent, too exact, and too internally coherent, leading paradoxically to a loss of felt realism. Individuals experiencing perceptual over-integrity do not report visual distortions, hallucinations, or sensory loss. Instead, they describe the world as unnaturally crisp, reliable, and unchanging. Objects appear exactly as they should, movements are predictable, and sensory input lacks fluctuation. This excessive regularity produces unease. The world feels correct, yet strangely lifeless. Patients often say, “Everything looks normal, but it doesn’t feel normal.” This condition differs from derealization, where the world feels unreal or dreamlike. In perceptual over-integrity, reality feels too real, too perfectly assembled. The problem is not detachment, but saturation of order. Normally, perception contains micro-variations, noise, and ambiguity that signal vitality. When these disappear, experience becomes static, as if perception has been frozen at maximum resolution. Phenomenologically, this state often triggers a sense of existential threat. The individual may feel that reality has lost its capacity to surprise or breathe. Time may feel oddly suspended—not slowed or sped up, but stabilized to the point of rigidity. This can produce anxiety not tied to danger, but to the suspicion that something fundamental has stopped moving. Neurocognitively, perceptual over-integrity may involve excessive top-down predictive control. The brain overconfidently predicts sensory input, leaving little room for novelty or error correction. As a result, perception becomes over-smoothed. This differs from psychosis, where predictions overpower sensory input and produce false perceptions. Here, predictions dominate without producing error—creating a world that is too perfectly anticipated. Clinically, this condition is difficult to articulate and often misunderstood. Because patients insist that nothing looks distorted, clinicians may dismiss the experience as philosophical or anxiety-driven. However, the distress is sensory and immediate. Individuals may avoid stillness, silence, or minimal environments where perceptual stability becomes more apparent. Movement, noise, or visual complexity may temporarily relieve symptoms by reintroducing variation. Behaviorally, individuals may seek stimulation not for pleasure, but to disrupt perceptual rigidity. Conversely, some may withdraw, fearing that interaction will intensify the uncanny stability of the world. Neither strategy addresses the core disturbance, which lies in the balance between predictability and surprise in perception. Treatment approaches are exploratory. Grounding techniques that rely on focusing on sensory detail may paradoxically worsen the experience, as detail is already excessive. Instead, interventions that reintroduce unpredictability—creative activity, improvisational movement, or environments rich in natural variability—may help restore perceptual elasticity. Pharmacological effects are inconsistent and poorly studied. Perceptual Over-Integrity challenges the assumption that realism increases with perceptual accuracy. This phenomenon suggests that lived reality depends not on perfect coherence, but on subtle instability. A world that is too well-assembled can feel just as unreal as one that is distorted. It reveals that mental health requires not only order, but flexibility—a perceptual field that can wobble slightly, allowing experience to feel alive rather than complete.
Intentionality Collapse
Most psychiatric models assume that thoughts are inherently intentional—that they are about something. A thought refers to an object, a memory, a fear, a plan, or a belief. Yet a rarely described disturbance exists in which thoughts continue to arise clearly and fluently, but lose their sense of aboutness. This phenomenon can be described as Intentionality Collapse, a condition in which cognition remains active while its directional structure quietly dissolves. Individuals experiencing intentionality collapse often report that their mind is “working,” “thinking,” or “producing language,” yet those thoughts no longer feel anchored to anything. The content may be grammatically coherent and logically formed, but internally it feels hollow, unpointed, or unmoored. A sentence appears in the mind, but it does not clearly refer to a concern, desire, or object in the world. The person may say, “Thoughts are happening, but they are not about my life.” This condition is not thought disorder in the psychotic sense. Speech remains organized, associations are intact, and reality testing is preserved. Nor is it dissociation, as consciousness remains vivid and present. The disturbance lies at a more fundamental level: the collapse of intentional structure that normally binds mind to world. Thoughts float without destination. Phenomenologically, this creates a profound sense of estrangement without detachment. The individual does not feel unreal or numb. Instead, they feel cognitively active but existentially disconnected. Planning becomes difficult not because of indecision, but because plans lack gravitational pull. Memories surface but fail to evoke relevance. Even worries may arise abstractly, stripped of urgency. This phenomenon differs from depression, where thoughts are often negative and self-referential. In intentionality collapse, the problem is not negative content but loss of reference. The self is not attacked; it is bypassed. Individuals often describe feeling “mentally verbose but existentially silent.” From a neurophenomenological perspective, intentionality collapse may reflect a disruption in integrative networks that bind semantic content to motivational and affective systems. The brain continues to generate representations, but fails to link them to value, agency, or concern. As a result, cognition becomes self-sustaining but self-detached. Clinically, this state is frequently misinterpreted as intellectualization, burnout, or philosophical rumination. Because patients can articulate their experience clearly, clinicians may underestimate the severity of the disturbance. Yet many individuals find this condition deeply distressing, as it undermines the basic function of thought as a tool for living. Thinking no longer helps one be in the world. Behaviorally, individuals may continue to function outwardly, responding appropriately to demands, yet feel increasingly alienated from their own actions. Choices feel arbitrary, not because values are absent, but because values no longer attach themselves to thought. Over time, this can lead to passivity, not from lack of will, but from loss of directional cognition. Treatment remains largely undefined. Insight-oriented approaches often fail, as the individual already understands the problem conceptually. Forcing meaning or narrative can worsen the sense of artificiality. Emerging observations suggest that intentionality may return not through reflection, but through embodied engagement—action before meaning, involvement before interpretation. Meaning reattaches itself only after the mind stops trying to generate it directly. Intentionality Collapse challenges a foundational assumption of psychology: that thinking naturally connects us to the world. This phenomenon suggests that cognition can persist in isolation, detached from concern, purpose, or reference. Mental suffering here does not arise from distorted beliefs or painful emotions, but from the quiet disappearance of direction itself. It reveals that what sustains human experience is not merely the presence of thought, but its orientation—its ability to point beyond itself. When that pointing collapses, the mind continues to speak, but no longer knows to whom or about what.
When Moral Weight Exists Without Emotion
In most psychiatric frameworks, guilt is understood as an affective state—painful, heavy, emotionally charged. It is commonly linked to depression, anxiety disorders, or obsessive–compulsive pathology. Yet a rarely described phenomenon exists in which guilt persists after emotion has disappeared. This condition, which may be termed Non-Affective Guilt, involves the experience of moral responsibility without accompanying emotional distress, remorse, or self-punishment. Individuals experiencing non-affective guilt do not feel sad, anxious, ashamed, or self-critical. Instead, they report a cold, persistent sense of having done something wrong or of being morally misaligned, even when no clear transgression can be identified. The guilt is not felt in the chest or gut; it is felt as a fact. Patients often say, “I know I’m guilty, but I don’t feel bad,” or “The guilt is there, but it has no emotion attached to it.” This phenomenon differs fundamentally from psychopathy or lack of conscience. Moral reasoning remains intact, sometimes even heightened. The individual understands ethical norms, recognizes responsibility, and may behave conscientiously. What is missing is the affective signal that normally accompanies guilt. This creates a disturbing split: moral cognition persists without emotional reinforcement, leaving the individual trapped in a state of unresolved responsibility. Non-affective guilt also differs from obsessive guilt, where anxiety drives compulsive reassurance or confession. Here, there is no urgency to neutralize the guilt, no panic, no intrusive fear. The guilt does not escalate—it simply remains. Its persistence is what makes it distressing. Patients describe it as “static,” “background,” or “structural,” as if guilt has become part of the architecture of consciousness rather than a passing feeling. Phenomenologically, this state can erode identity. Emotion normally allows guilt to resolve—through remorse, apology, forgiveness, or self-compassion. Without emotion, resolution becomes impossible. The individual may repeatedly review past actions, not to relieve anxiety, but to locate the source of an ever-present moral imbalance. When no source is found, the guilt becomes existential rather than situational. Neuropsychologically, non-affective guilt may reflect a decoupling between moral evaluation systems and affective processing networks. The brain continues to generate judgments of responsibility but fails to translate them into emotional experience. This decoupling can occur after prolonged depression, emotional numbing, trauma, or certain pharmacological interventions, yet it often persists even after mood and anxiety symptoms resolve. Clinically, non-affective guilt is frequently misunderstood or ignored. Because patients do not appear distressed in conventional ways, clinicians may assume the guilt is mild or philosophical. In reality, the suffering lies in moral paralysis. The individual cannot feel absolution, relief, or closure, because these experiences are emotionally mediated. Guilt becomes infinite not because it is intense, but because it cannot complete its cycle. Treatment poses a unique challenge. Cognitive reassurance fails, as the person already understands that their guilt may be irrational or unfounded. Emotional processing techniques may also fail, because the emotional channel is inaccessible. Some emerging approaches focus instead on embodied moral repair—action, restitution, and ethical alignment in the present rather than emotional resolution of the past. The aim is not to feel forgiven, but to live in a way that gradually dissolves guilt through lived coherence. Non-Affective Guilt challenges a core psychiatric assumption: that moral suffering requires emotional pain. This condition demonstrates that guilt can survive the disappearance of feeling and continue to shape consciousness as a silent, unresolved weight. It suggests that morality is not only emotional, but structural—and that healing may sometimes require restoring the emotional dimension, not to intensify guilt, but to allow it to finally end.
Deferred Recognition of Return
The final stage in the trajectory that begins with Irreversibility Anxiety and passes through silent reconstruction is not marked by a change in consciousness itself, but by a change in awareness of change. This phase can be described as Deferred Recognition of Return. It occurs when the individual realizes—often suddenly, often accidentally—that they have already returned, even though no moment of return was ever felt. The defining characteristic of this stage is temporal displacement. Recovery is not experienced in the present tense. It is recognized only after the fact. A person may recall a recent conversation, decision, or emotional reaction and notice something quietly shocking: “I didn’t check myself,” “I didn’t worry whether this would last,” or “I moved on without noticing.” The realization does not feel euphoric. It feels oddly neutral, even understated, yet deeply grounding. Unlike conventional recovery narratives, there is no sense of triumph or closure. The mind does not declare itself healed. Instead, it encounters evidence—scattered, unannounced—that flexibility has already returned. The ability to leave mental states, once feared lost forever, is now functioning again, but without self-reference. The psyche did not come back; it resumed. Phenomenologically, this stage involves a restoration of background trust. The individual no longer experiences consciousness as something that must be protected, monitored, or stabilized. Thoughts can deepen without fear of entrapment. Emotions can intensify without signaling danger. Even difficult states are tolerated differently—not because they are pleasant, but because they are no longer interpreted as final. Importantly, this trust is not a belief. It is a felt assumption that operates beneath reflection. This phase differs from insight-driven healing. Understanding what happened may still feel incomplete or abstract. Some individuals never fully articulate the experience that once dominated their lives. Yet this lack of narrative does not impair functioning. In fact, the absence of a complete explanation often protects the regained flexibility. The mind no longer needs to know why it survived in order to live normally again. A striking feature of Deferred Recognition of Return is grief without pathology. Many individuals experience a subtle mourning—not for suffering, but for the self that once believed in irreversible collapse. There may be sadness for the time spent waiting, monitoring, or fearing. Yet this grief is not destabilizing. It unfolds within a mind that now knows, implicitly, that states pass. Clinically, this stage is frequently invisible. Patients may discontinue therapy not because they are cured, but because the question that brought them there has dissolved. Others may remain in treatment while struggling to explain why their distress no longer feels urgent. Clinicians unfamiliar with this trajectory may misinterpret the absence of dramatic relief as incomplete recovery, when in fact the deepest repair has already occurred. Perhaps the most important feature of this stage is that it resists ownership. The individual cannot clearly say, “I recovered.” There is no method to credit, no moment to point to, no insight to preserve. This lack of ownership is precisely what stabilizes the return. The mind has relearned that it does not need to supervise its own continuity. Deferred Recognition of Return reveals a final, quiet truth about certain forms of psychological collapse: the fear of irreversibility is resolved not by proving reversibility, but by living long enough for reversibility to reassert itself without comment. What once felt like a point of no return becomes, in retrospect, a passage that never announced its exit. In this way, recovery does not arrive as an event, but as an absence—the absence of vigilance, the absence of checking, the absence of the question, “Am I still stuck?” And in that absence, life resumes its most basic function: moving forward without needing to know that it can.
Chronotaraxis
Chronotaraxis is an uncommon neuropsychiatric disturbance characterized by a profound disruption in the subjective ordering of time, in which past, present, and future lose their normal sequential structure. Unlike generalized memory impairment, chronotaraxis involves a selective breakdown in temporal coherence while episodic content remains relatively preserved. Neurobiologically, the condition reflects dysfunction within distributed cortico–hippocampal–striatal networks that normally encode temporal context and enable the continuous flow of conscious experience. The hippocampus plays a central role in temporal binding by organizing discrete experiences into sequential frameworks. Damage to hippocampal subfields, particularly CA1, impairs the encoding of temporal order without necessarily erasing the events themselves. This dissociation explains why individuals with chronotaraxis may accurately recall specific experiences yet be unable to place them within a meaningful timeline. The disruption extends beyond memory storage, implicating hippocampal interactions with the entorhinal cortex, where time cells and grid-like temporal representations contribute to the brain’s internal chronometric system. Prefrontal regions, especially the dorsolateral and medial prefrontal cortex, are essential for maintaining temporal continuity across working memory and long-term representations. Lesions or functional hypoconnectivity in these areas reduce the capacity to stabilize a “now” state, resulting in a fluctuating or fragmented present moment. Within this framework, conscious awareness becomes temporally unstable, as the brain fails to anchor ongoing perception to a coherent temporal reference point. Basal ganglia and cerebellar contributions further modulate temporal precision. The striatum, through dopaminergic signaling, supports interval timing and the prediction of event durations. Dysregulation within frontostriatal loops can distort subjective time estimation, leading to experiences in which seconds may feel interminable or collapse instantaneously. When combined with hippocampal temporal disorganization, these distortions produce the characteristic phenomenology of chronotaraxis: time is experienced not merely as fast or slow, but as structurally disordered. From a network perspective, chronotaraxis involves impaired coordination between the default mode network and the salience network. The default mode network generates autobiographical continuity, while the salience network identifies the relevance of present-moment stimuli. When their interaction is disrupted, internally generated temporal narratives dominate over external temporal cues. This imbalance allows memories to intrude into the present with the vividness of current perception, blurring the boundary between recollection and immediacy. Predictive processing models conceptualize chronotaraxis as a failure to maintain hierarchical temporal predictions. Normally, the brain anticipates the near future and continuously updates these predictions based on sensory input. In chronotaraxis, high-level temporal priors become unstable or overly permissive, allowing multiple temporal hypotheses to coexist. The resulting conscious experience lacks a privileged present, giving rise to the subjective sense that time itself has lost direction. Clinically, chronotaraxis is most often observed following right hemisphere lesions, traumatic brain injury, or in certain neurodegenerative conditions, yet it remains underrecognized due to its subtle and introspective nature. Patients may struggle to articulate their experience, describing instead a sense of being “unstuck” from time. This phenomenological elusiveness has contributed to its marginal presence in psychiatric classification systems. As a neurobiological phenomenon, chronotaraxis highlights the active construction of temporal experience by the brain. It demonstrates that time, as lived and perceived, is not a passive dimension but an emergent property of coordinated neural dynamics. When these dynamics falter, the brain does not simply lose track of time—it reorganizes experience into a temporally fragmented reality that challenges conventional distinctions between memory, perception, and anticipation.
Somatoparaphrenia
Somatoparaphrenia is a rare neuropsychiatric condition in which patients deny ownership of a limb or an entire side of their body, despite intact primary sensory input and preserved intellectual awareness. Neurobiologically, the syndrome reflects a breakdown in multisensory body representation rather than a deficit in somatosensation per se. Lesion and functional studies consistently implicate the right inferior parietal lobule, temporoparietal junction, and insular cortex, regions critical for integrating proprioceptive, tactile, visual, and interoceptive signals into a unified sense of bodily self. The parietal cortex plays a central role in constructing the body schema by continuously updating the spatial and relational properties of body parts relative to one another and to external space. In somatoparaphrenia, damage to the right parietal network disrupts this updating process, leading to a fragmentation of bodily representation. The affected limb remains perceptually accessible but is no longer incorporated into the egocentric body model. This dissociation suggests that body ownership is not an inherent property of sensory input but an inferential product of cortical integration. The insular cortex contributes a crucial affective and interoceptive dimension to body ownership. By mapping internal physiological states and associating them with bodily boundaries, the insula anchors the body schema to a subjective sense of “mineness.” When insular–parietal connectivity is compromised, the limb may be represented spatially but lacks the interoceptive signature required for ownership attribution. This mechanism helps explain why patients may acknowledge that a limb is attached to their body while simultaneously insisting that it belongs to someone else or is entirely foreign. Frontal regions, particularly the right ventromedial prefrontal cortex, modulate belief evaluation and self-related attribution. Lesions in these areas reduce the capacity to reconcile contradictory information, allowing implausible interpretations of bodily experience to persist. Within predictive coding models, somatoparaphrenia can be understood as a failure to resolve prediction errors between expected bodily states and incoming sensory data. Rather than updating the internal body model, the system externalizes the discrepancy, attributing the limb to an external agent or denying its existence altogether. Neuroimaging evidence suggests abnormal functional coupling between the default mode network and salience network in somatoparaphrenia. The default mode network, involved in self-referential processing, generates an internally coherent narrative of bodily identity that excludes the affected limb. Simultaneously, impaired salience signaling prevents the anomalous sensory evidence from gaining sufficient weight to challenge this narrative. The result is a stable delusional belief that resists correction even in the face of direct visual and tactile confrontation. Clinically, somatoparaphrenia differs from anosognosia in that the deficit is not a simple lack of awareness but an active misattribution of ownership. The emotional tone associated with the disowned limb can range from indifference to hostility, reflecting partial preservation of affective processing coupled with distorted self-representation. This emotional variability further supports the view that the disorder arises from disrupted integration rather than global emotional blunting. From a broader neuroscientific perspective, somatoparaphrenia illuminates the constructed nature of bodily self-consciousness. It demonstrates that the sense of owning a body is not localized to a single cortical area but emerges from dynamic interactions among parietal, insular, and frontal networks. When these interactions are selectively impaired, the brain does not merely lose the body—it reinterprets it, generating alternative explanations that preserve internal coherence at the expense of objective reality.
Reduplicative paramnesia
Reduplicative paramnesia is a rare neuropsychiatric phenomenon characterized by the persistent delusional belief that a familiar place, person, or object has been duplicated and exists simultaneously in multiple locations. Unlike more widely discussed misidentification syndromes, reduplicative paramnesia occupies an ambiguous position at the intersection of psychiatry, neurology, and cognitive neuroscience, resisting simple classification as either a purely delusional disorder or a straightforward consequence of focal brain injury. The condition is most frequently observed following lesions to the right frontal or parietal lobes, yet its phenomenology cannot be fully explained by structural damage alone, suggesting a more complex disturbance in the integration of memory, spatial representation, and belief evaluation. Patients with reduplicative paramnesia often demonstrate a striking paradox: while their general cognitive functioning may appear relatively preserved, they exhibit an unshakeable conviction that a particular place—such as a hospital, home, or city—exists in two or more identical copies. Importantly, this belief is not merely a transient confusion or confabulation but a stable and elaborated delusional system, frequently defended with elaborate rationalizations. Attempts to correct the belief through logical argument or sensory evidence typically fail, highlighting a disruption not in perception itself but in the mechanisms responsible for reality monitoring and belief updating. From a neurocognitive perspective, reduplicative paramnesia has been associated with impairments in the binding of contextual memory and emotional familiarity. The patient may correctly recognize a location at a perceptual level, yet experience a mismatch between the expected emotional or autobiographical resonance of that place and the present sensory input. This dissonance appears to be resolved through delusional duplication, allowing the individual to preserve both perceptual recognition and the subjective sense that “something is wrong.” In this sense, the delusion may function as a compensatory narrative rather than a random psychotic production. Clinically, reduplicative paramnesia presents a challenge for differential diagnosis. It can resemble psychotic disorders, particularly delusional disorder or schizophrenia, yet it often emerges abruptly following neurological insult and lacks the broader thought disorder or hallucinations typical of primary psychosis. Conversely, when it appears in the context of neurodegenerative disease or traumatic brain injury, its persistence and thematic specificity distinguish it from generalized confusional states such as delirium. This diagnostic ambiguity has contributed to its relative neglect in both psychiatric and neurological literature. Treatment approaches remain largely empirical. Antipsychotic medications have shown inconsistent efficacy, particularly when structural brain damage is prominent. Cognitive and environmental interventions, aimed at reducing stress and minimizing confrontations over the delusional belief, appear to be more beneficial in maintaining functional stability. The limited responsiveness to pharmacological treatment further supports the view that reduplicative paramnesia reflects a disorder of belief formation rather than a classic dopaminergic psychosis. Theoretical interest in reduplicative paramnesia extends beyond its clinical rarity. The syndrome offers a unique window into the mechanisms by which the human brain constructs a coherent sense of place and continuity. Its existence challenges simplistic models of delusion as mere false beliefs and instead points toward a breakdown in the dynamic negotiation between perception, memory, affect, and executive control. As such, reduplicative paramnesia occupies a disproportionately important role in discussions about the nature of reality testing and the fragile architecture underlying what is ordinarily experienced as a stable world.
Truman Show Delusion
Truman Show Delusion is a rare and culturally influenced delusional disorder in which individuals become convinced that their lives are secretly being observed, recorded, or broadcast to an audience. Unlike classical persecutory delusions that focus on direct harm or threat, this syndrome is distinguished by the perception that one’s existence has been transformed into a form of entertainment or a controlled experiment. Ordinary environmental occurrences—such as media broadcasts, public conversations, or coincidental encounters—are interpreted as deliberate signals orchestrated by external agents, reinforcing the belief that reality itself is scripted. The delusion often draws inspiration from popular culture, notably films depicting life as a monitored or artificial construct, highlighting the interplay between media exposure and psychopathology. The disorder centers on a profound disruption of self-referential processing. Individuals perceive themselves as the central focus of all external events, transforming neutral or unrelated stimuli into personally meaningful signs. This heightened sense of personal significance generates pervasive hypervigilance, paranoia, and a constant search for hidden messages. Patients report meticulously analyzing interactions, environmental cues, and social behaviors to detect patterns, often exhausting themselves in the process. The blurring of internal thought and external reality can also produce intrusive rumination, emotional dysregulation, and chronic anxiety, as the individual experiences a continuous threat to personal privacy and autonomy. Neurological and cognitive factors are believed to contribute to the emergence of Truman Show Delusion. Dysfunctions in brain regions responsible for reality monitoring, such as the prefrontal cortex, anterior cingulate, and parietal lobes, may impair the ability to differentiate between internally generated thoughts and external events. This deficit is compounded by hyperactivity in self-referential networks and aberrant salience attribution, causing ordinary stimuli to acquire exaggerated personal significance. In addition, comorbid psychiatric conditions—including schizophrenia, bipolar disorder, or severe anxiety disorders—appear to increase susceptibility, providing a fertile ground for culturally shaped delusional beliefs to take hold. The social and emotional consequences of Truman Show Delusion are profound. Patients frequently withdraw from interpersonal contact, fearing observation or manipulation, and may become distrustful of family, friends, and even medical professionals. Sleep disturbances, irritability, and depressive symptoms commonly accompany the delusion, as the constant perception of being monitored generates persistent psychological strain. In some cases, the individual may attempt to test the boundaries of reality through elaborate behavioral experiments, which can exacerbate both risk and distress. The condition thus exemplifies the intersection of cognitive distortion, affective dysregulation, and sociocultural context, demonstrating how modern media and personal identity interact to shape psychopathology. Treatment remains challenging due to the syndrome’s rarity and complex etiology. Antipsychotic medications targeting dopaminergic pathways can reduce delusional intensity, while cognitive-behavioral approaches aim to restore reality testing and reduce hypervigilance. Psychoeducation about the cognitive mechanisms underlying self-referential distortion and cultural influence is also essential to promote insight. Early intervention, combined with supportive therapy, appears to improve functional outcomes, although some patients experience persistent residual paranoia or mistrust. Truman Show Delusion highlights the fragility of human perception and the intricate interplay between cognition, culture, and identity. By illustrating how ordinary environmental stimuli can be transformed into personalized narratives of surveillance, the syndrome offers critical insight into the neural and psychological mechanisms underpinning reality monitoring, selfhood, and the human need for control over one’s own life. It underscores the delicate balance between personal meaning-making and the potential for affective and cognitive overload, demonstrating that modern cultural narratives can profoundly shape the content and expression of psychopathology.
Foreign Accent Syndrome
Foreign Accent Syndrome is a rare neuropsychological condition in which individuals suddenly begin to speak their native language with a perceived foreign accent, despite having no prior exposure to or proficiency in the accent in question. The phenomenon does not involve the acquisition of a new language but rather a disruption in the motor planning and prosodic features of speech, such as intonation, rhythm, and phoneme articulation. This alteration most commonly follows neurological events including stroke or traumatic brain injury, although psychiatric origins have also been documented. Beyond its neurological basis, Foreign Accent Syndrome carries significant psychological consequences. Speech functions not only as a means of communication but also as a fundamental component of personal and cultural identity. When the familiar sound of one’s own voice becomes altered, individuals often experience a sense of alienation and loss of self-coherence. Patients frequently report that their speech feels externally imposed, despite remaining cognitively intact. Social interaction further intensifies this psychological disturbance. Listeners often attribute the accent to foreign origin, which can lead to misunderstanding, stigmatization, or disbelief when the individual denies any connection to the perceived accent. This mismatch between internal identity and external perception generates emotional distress, contributing to anxiety, social withdrawal, and depressive symptoms. At a deeper level, the syndrome exposes the instability of linguistic identity. It demonstrates that the sense of self is partially constructed through unconscious motor and auditory feedback mechanisms rather than deliberate intention. A subtle neurological disruption can therefore produce profound changes in self-perception without altering personality, memory, or intelligence. Foreign Accent Syndrome challenges the traditional separation between neurological and psychological disorders. It illustrates how minimal changes in speech production can destabilize personal identity and social belonging, revealing the extent to which the self is embedded in bodily and linguistic processes beyond conscious control.
Stendhal Syndrome
Stendhal syndrome represents a rare yet striking psychological reaction in which intense exposure to aesthetic beauty precipitates a cascade of emotional and cognitive disturbances. The condition unfolds primarily through affective mechanisms rather than structural psychopathology, beginning with an overwhelming sense of awe that exceeds the individual’s emotional regulatory capacity. This initial state of admiration and reverence, typically associated with positive psychological growth, becomes destabilizing when sensory, symbolic, and cultural stimuli converge at an intensity that cannot be cognitively integrated. As emotional saturation increases, the individual experiences a loss of internal equilibrium, leading to heightened autonomic arousal and the emergence of anxiety. Physiological responses such as tachycardia, dizziness, and somatic discomfort accompany a subjective sense of losing control, transforming the aesthetic encounter from a source of pleasure into a perceived psychological threat. In response to this escalating distress, dissociation often emerges as a defensive strategy, manifesting as depersonalization, derealization, or emotional numbing, through which the psyche attempts to attenuate overwhelming affect by creating perceptual and emotional distance. During this phase, reality may appear distorted or unreal, not as a result of psychosis but as a consequence of affective overload disrupting perceptual coherence. In some individuals, the experience extends beyond immediate emotional dysregulation into existential disorientation, characterized by confusion regarding personal identity, meaning, and human limitation when confronted with transcendent beauty. This confrontation may evoke feelings of insignificance and vulnerability, destabilizing the sense of self rather than enriching it. Although symptoms typically subside once the individual is removed from the triggering environment, residual emotional effects may persist, including heightened sensitivity, fatigue, or ambivalence toward future aesthetic experiences. Viewed through this affective lens, Stendhal syndrome illustrates that psychological disturbance can arise not from negative stimuli alone, but from the collapse of emotional regulation under excessive positive intensity, thereby offering critical insight into the fragile boundaries of human emotional tolerance and perceptual stability.